WARNING! THIS POST CONTAINS GRAPHIC IMAGES.
*Please note, names have been changed to protect our patient’s identity
On the western coast of Sierra Leone, near Tagrin Bay, one of the most photogenic landscapes I have ever seen, Sierra Leone’s capital, Freetown, bustles with the sounds of Okada motorbikes speeding down streets, honking vehicles rushing to climb the city’s steep inclines. Friends yell, laugh, and share joy. But on the morning of November 6th, 2021 the city fell silent as the devastation of the night before gripped the city in its unforgiving jaws of reality.
A tanker full of petrol – struck by a large truck – was leaking onto the city streets. Seizing the opportunity of free fuel, onlookers started to gather as much petrol as possible. Others, some watching the chaos unfold, some stuck in the traffic backed up from the collision, suddenly became victims of one of the country’s largest tragedies.
Nearly 100 bodies lay charred, exposed, and lifeless on this, now sombre, city street. Approximately 200 others were rushed to receive immediate burn care at Freetown’s, now exceedingly overwhelmed, hospitals. Spread over more than 5 hospitals, as both in and out-patients, Sierra Leone’s healthcare system had to manage the impossible.
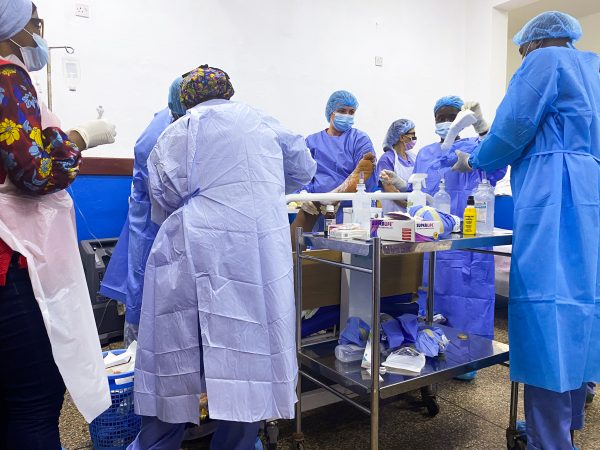
I arrived in Sierra Leone two weeks after the accident as part of Global Response Medicine’s team, comprised of a burn surgeon, several burn nurses, critical care providers, and administrative staff. We worked to help the local hospitals, still overrun by critical burn patients, navigate their treatment and management – many of whom now fiercely aware of a third cause of burn deaths – infection.

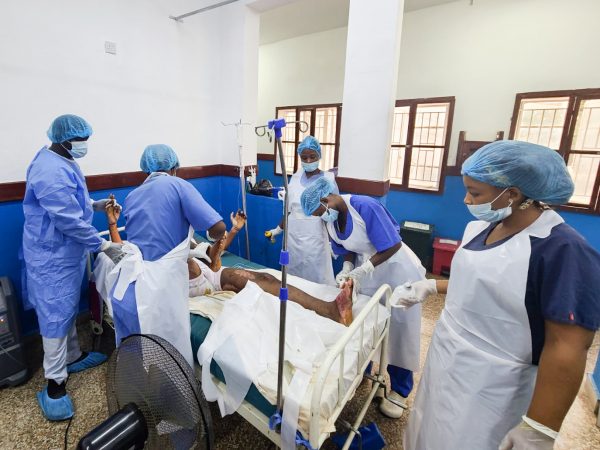
While the details of the patients and their conditions can be more eloquently shared by those who provided “hands-on” patient care, the logistics of the situation were heavy on my shoulders. This is an excerpt of my writings in real time, both from notes and reflective journaling while in Freetown:
Nov. 22nd :
- Burn care and dressing changes started at appx. 11 a.m.. Screams from suffering patients are almost unbearable. For hours, while dressings are changed, eschar is lifted, as they plead for their turn to be over. Worked with logisticians to plan buildout of makeshift operating room.
- paracetamol is the most common pain medication administered – ketamine and other narcotics are extremely scarce and used extremely judiciously.
- Female with severe leg burns are infected, combined with a lack of adequate amounts and variety of antibiotics, bilateral below-the-knee amputation is likely the only measure left for preservation of life.
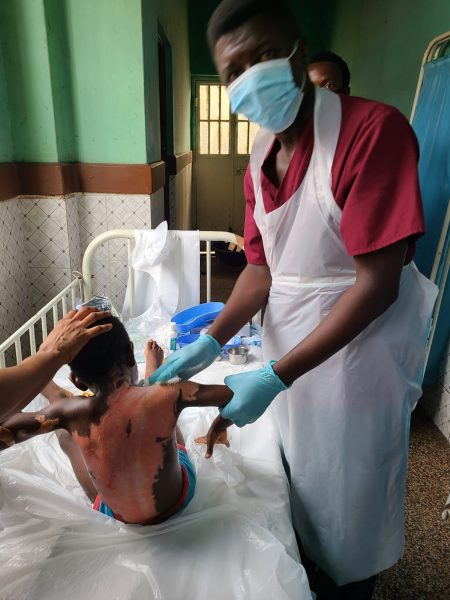
Nov 23rd: Progress is made on the idea of a standalone OR [“operating room”]. Lead physician at Military 34 Hospital approves tour of OR for our team to get an idea of what supplies they can help provide. Staff warns us: “it’s not much”.
Nov 23rd: GRM meets with team at public local hospital. There is a male patient who has opted out of further care, wounds are so infected and dressings are dried into the wounds; patient has settled with the idea of death.
Nov 24th: tour of OR complete. No AED/defibrillator in OR. Only a 3 lead and a disposable pulse ox probe noted on cardiac monitor. Bovie is reported to be in good working condition. Note a bucket of rust colored endotracheal tubes near scrub sink – local physician reports they are reused until they can no longer be reused as supply of such material is very short (shortage is not unique to the burn incident).
Personal diary entry at end of Nov 27th: Today we cared for an adolescent female who had over 80% 3rd degree burns. How she is alive still, I will never know. Most of her extremities are exposed muscle. She continues to blink and cry as we change her dressings; there isn’t enough ketamine available to make her more comfortable. When we are done, she is wrapped in burn dressings, literally from head to toe. Speaking of, several of her toes have been lost due to infection/necrosis. I have honestly never seen anything so devastating. I remain inspired by her will to live, her perseverance, and her faith in her providers.
Nov 29th: Young female passed away.
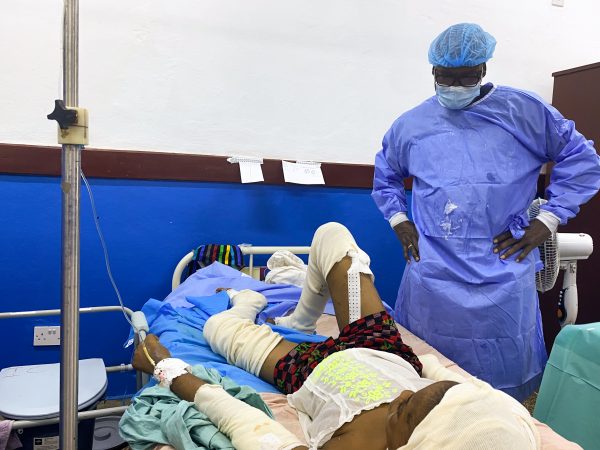
When the world seems overwhelming:
Overlooking the bright lights of Paris on a red-eye, midnight flight, I remain exhausted and emotionally taxed from my experience. I am headed back to my primary project in Matamoros, Mexico, where for the last year I have been fussing about the incredible lack of resources we have access to in order to treat our patients. As I watch the lights of Paris escape behind the wing of the plane, I realize I would give anything to have brought the short supply of resources from Mexico with me to Sierra Leone. Would it have made much of a difference? I guess we will never know, but science makes me believe the answer is a resounding YES.
As a man who has never been accused of being under-sensitive, I think back to the lesson that has helped me manage the rollercoaster of emotions and feelings that a life in healthcare has presented; I didn’t cause tragedy and my only responsibility is to do my part to make it better. And then I repeat what I recite every morning; “Do not be daunted by the enormity of the world’s grief. Do justly now, love mercy now, walk humbly now. You are not obligated to complete the work, but neither are you free to abandon it.” (The Talmud)
So many of us in healthcare rely on that or something similar to get through. I say get through as a blanket statement; to get through our shift, to get through the week, to get through the code, the funeral, our careers. How many of us are actually taking that to heart? Do we really not carry the entire weight of the world’s grief on our shoulders? How much of what we experience are we willing to let go of in order to be healthy; not just physically but mentally.

Is love the secret?
I wish I had the secret, but the stern reality is that I do not. In fact, I may be farthest away from having it. I do know one thing, though, and it was never more prominent than my experience in Sierra Leone:
There are many factors to the human condition. The one that tends to cure me the most, however, is the expression of love.
I spent nearly two years in Matamoros as the project manager, and through it all, the one thing that was never lacking was love. Love for humans. Love for medicine. Love for justice and equity. Love for mercy. Love for a better tomorrow. Love for a child’s laughter. Love for a good prognosis or a successful treatment. Love for one another.
The love that pressed on my soul as an impression of my experience in Sierra Leone made me a better project manager, a better friend, a better father, and a better human. I am immensely grateful for GRM and their ability to plug into situations where love is needed the most. Where we can go and do things no one else can do. That we have the opportunity to create more of those tiny pieces of paper that not only help cover and heal the pain of our patients, but that those metaphorical pieces of paper also begin to heal our own pain.
When it comes to what we need the most, I am forever grateful for what the people of Sierra Leone and Matamoros, Mexico have taught me: love heals and love wins.
BLOG POSTS ARE THE OPINION OF THE AUTHOR AND DO NOT NECESSARILY REPRESENT THE VIEW OF GRM